Blog
Jan 17, 2023
5 Ways for Healthcare Providers to Unlock the Benefits of Telehealth

With four out of every five rural counties in the United States lacking psychiatric care, members of rural regions end up relying on larger neighboring towns to access these services. In 2017 alone, 60 million Americans went without treatment for a mental illness, undoubtedly the requirement to travel long distances to receive care contributed to that statistic.
Over the last several years, however, the increasing availability of virtual psychiatry services has broken down geographic barriers and expanded access to mental health care. More broadly, telehealth, which refers to healthcare services delivered using technology such as video, email, text, and cell phone applications, has become a crucial tool for providers of ambulatory care, private practice medical practitioners, and hospitals.
Before the COVID-19 pandemic, telehealth was rarely used and often distrusted by both patients and physicians as a way of providing healthcare. The limitations of the pandemic, however, meant that 75% of hospitals were providing telehealth services by June of 2020. Additionally, the Centers for Medicare & Medicaid Services expanded the list of reimbursable telehealth codes for the 2021 physician fee schedule, making it more feasible for publicly insured individuals to pay for telehealth appointments and services. Because of this, a significant set of patients were encouraged to try telehealth, with the majority finding it highly convenient and showing an interest in utilizing it moving forward. In fact, virtual visits rose by 78 times from February to April 2020 and remained at 38 times prior levels in mid-2021.
In envisioning the future of healthcare, telehealth is anticipated to continue playing a vital role to bridge patients to their providers. Telehealth currently makes up 13-17% of all medical services and is projected to grow from a market size of $90 billion in 2021 to over $600 billion in 2028, representing a compound annual growth rate (CAGR) of over 30%. Additionally, investors put $30 billion toward telehealth startups in 2021.
It is crucial that each provider individually examines the ways in which telehealth could enhance their healthcare services. When utilized properly, telehealth becomes an invaluable tool for making healthcare more efficient, convenient, and equitable.
The Benefits of Telehealth
The advantages of telehealth extend to nearly all sectors of healthcare. Virtual visits can be more cost-effective and convenient than in-person visits, while also reducing the spread of transmissible diseases. Combined with the rising availability of remote health monitoring technology, telehealth can also help lay the groundwork for a more personalized healthcare experience. The below image provides more details on our perspective regarding the advantages of telehealth for both healthcare professionals and patients.
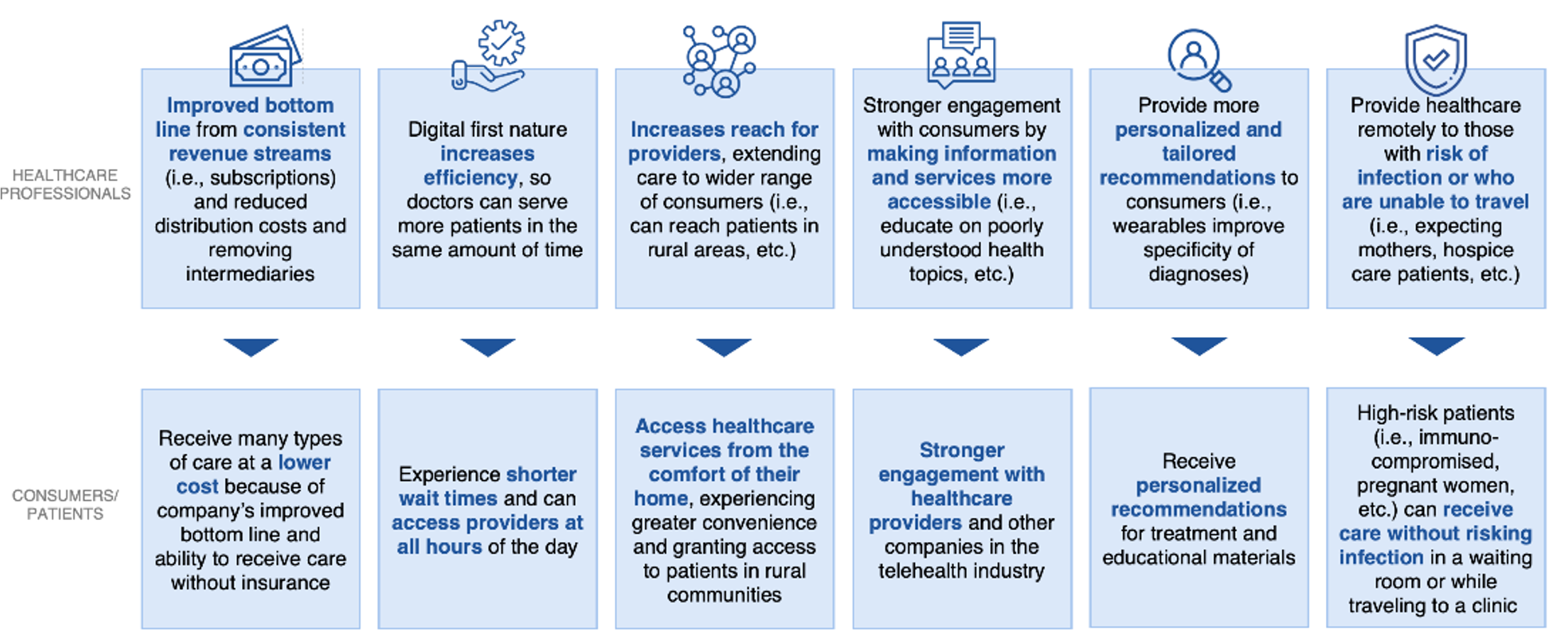
Six advantages of telehealth for healthcare professionals and patients
On a larger scale, telehealth has the potential to bring greater equity to healthcare. Patients living in areas that lack the physical presence of medical care and mental health support are now able to access a greater variety of these services virtually. However, access to technology needed to participate in telehealth and education on telehealth remains a barrier. Providers must keep in mind that populations who may benefit most from telehealth, such as the elderly or rural residents, may need additional support to learn about and access these services.
Unlocking the benefits of telehealth requires a unique approach that will vary based on provider, patient profile, cost, and more.
How Telehealth Can Be Implemented Today
Implementing telehealth can be a complex and daunting task. These five concrete steps provide a foundation for transforming your healthcare practice with telehealth:
1. Utilize a Hybrid Approach: Using a combination of in-person and virtual visits can allow a practice to reap the benefits of telehealth while filling in the gaps it can create. For example, after an initial physical therapy visit for an elderly person, follow-up meetings can be done virtually to reduce the strain and time cost of travel. Additionally, brief diagnostic calls for acute conditions can act as a screen to reduce the workload of overwhelmed emergency rooms, while also encouraging patients to seek care who might otherwise be hesitant to make the effort of an in-person visit.
2. Consider value-based care models: A key element of modern healthcare is redefining the measurement approach to the long-term outcome of patients over a fee-for-service model. Providers can maintain revenue through subscription-based telehealth services offering routine virtual primary care visits, which can catch medical issues early on and result in lowered medical costs of reactive long-term care.
3. Reflect patients’ needs: Rather than applying a blanket telehealth solution, providers should consider the telehealth offerings that can support their patient needs and requests. For example, a rural practice could transition to offering telehealth by first providing educational materials and overviews to make sure patients are aware of the benefits and availability of telehealth services.
4. Integrate remote monitoring: The increasing availability of remote monitoring technology enables metrics like vital signs or blood sugar levels to be assessed at home and made immediately available to physicians for interpretation. This can be useful for care centered around long-term tracking of chronic conditions. Continuous availability of a diabetic patient’s blood sugar levels, for example, allows a physician to create and adjust an individualized nutrition plan.
5. Assess digital capabilities: Generally, a successful implementation of telehealth requires practices to modernize the technology they use. This could include selecting a virtual conferencing service or preparing digital infrastructure to handle new sources of patient data. In addition to being functional, technology needs to be accessible and easy to use for both patients and physicians in order to realize the potential of telehealth as an efficient and convenient option.
Telehealth has been a key priority for the country’s largest healthcare providers, such as CVS Health’s Connected Care, UnitedHealth Group’s virtual primary care, therapy, and specialty visits, and Cigna’s virtual offerings for minor medical issues, dental counseling, and psychiatry. Major hospital networks like HCA Healthcare, CommonSpirit Health, and Encompass Medical Group offer a wide variety of virtual healthcare options as well. In the pharmaceutical sector, AstraZeneca is pursuing digital health initiatives with telehealth company Huma, and Emmaus Life Sciences has partnered with telehealth company UpScript to provide same-day physician authorization and prescription of a drug to treat sickle cell anemia.
Telehealth Assessment with Credera
In 2022, Credera worked with a large multinational pharmaceutical company to assess their current telehealth capabilities and identify a third-party telehealth service to meet their needs. Credera determined that a hybrid telehealth offering would best suit the company’s customer base and current offerings, which spanned chronic and acute care across multiple specialties. The selected vendor partner also needed to meet requirements for capabilities including connection with pharmacies, intelligent referrals, and the ability to share health metrics using third-party medical devices.
Credera identified several vendor partners that could meet the requirements, which led to a detailed analysis to generate and compare benefits and drawbacks for each partner until a final recommendation was determined. Ultimately, Credera recommended a partner with established market share, a variety of comprehensive offerings, and a far-reaching brick-and-mortar presence to support increased availability and visibility.
Have questions on how to improve or start using telehealth?
Credera can help assess how to improve the integration of telehealth into provider ecosystems and how various technologies or vendors can support that based on key use cases. Contact us at marketing@credera.com to learn how we can work together to accomplish your goals.
Contact Us
Let's talk!
We're ready to help turn your biggest challenges into your biggest advantages.
Searching for a new career?
View job openings





